This website was created as an assignment for Genetics 564 at the University of Wisconsin-Madison
|
What is CPVT? Catecholaminergic Polymorphic Ventricular Tachycardia or CPVT is a genetic heart arrhythmic condition that occurs in 1 out of 10,000 people. CPVT is caused by an irregular uptake of calcium by cardiac muscle cells or myocytes [1,2]. Calcium is an important element necessary for normal cardiac muscle contraction and regulation of it is disrupted in CPVT. People with CPVT have a mutation(s) in their RYR2 gene which as a result, creates a defective variant of the Ryanodine Recpector 2 protein, the protein responsible for regulating calcium ions in cardiac tissue[3,4]. As the name suggests, CPVT specifically affects the contraction of the ventricles or the lower chambers of the heart that are responsible for pumping blood to the lungs and the entire body. In CPVT, the ventricles of the heart are pumping faster than the atria or the top chambers of the heart. Because the heart is not pumping efficiently, a person with CPVT will often experience dizzy spells or fainting during exercise or situations of intense emotion or stress [1,2,3]. Though many arrhythmic episodes pass, CPVT is much more dangerous than other types arrhythmic disorders because the ventricular tachycardia can often transform into ventricular fibrillation. |
Animation 1: This animation demonstrates normal heart pumping function[9].
|
If this happens, the heart contracts sporadically and no blood is being pumped to the body which results in death if not treated immediately[2]. Unfortunately, in many cases, ventricular fibrillation is the first noticed symptom in people with CPVT and as a result there is a tendency for people with CPVT to die at a very young age without even knowing they had the disorder. If the cause of death is determined to be CPVT, family members are able to get genetically tested. Due to the fact that many people unknowingly have the defective gene and pass it down to their children, the disorder is highly lethal. It is estimated that over 30% of people with CPVT die from cardiac arrest or fibrillation before the age of thirty[3].
Diagnosis and Treatment
CPVT is an autosomal dominant genetic disorder. This means that if one parent has the disease, each of their children have a 50% chance of having the disease as well[2]. Sadly, the majority of people who get diagnosed with CPVT only get tested because an otherwise completely healthy relative suddenly died and it was later determined the cause of death was CPVT. People with CPVT have no symptoms that can be identified visually such as a structural heart defect, a trait of CPVT that prevents doctors from being able to identify the disorder by performing an echocardiogram[2,6]. The problem is at a molecular level. To determine if a person has CPVT, a Treadmill Stress Test is typically given. Since symptoms of CPVT are only expressed during exercise or moments of intense emotion, the arrhythmia is not present at a resting heart rate. Doctors need to elevate the heart rate to 120 beats in order to perform an electrocardiogram (ECG) for CPVT testing. As the heart rate climbs, doctors search for additional beats from the ventricles between atrial contractions. These are known as premature ventricular contractions[2]. These extra contractions can help doctors determine if CPVT is the diagnosis. Genetic testing is also a very common way for determining if one has CPVT. Genetic testing is very important step in diagnosis for families since the disorder is hereditary. Today, three genes have been identified for causing CPVT: RYR2, CASQ9 and TRND [2,6]. A mutation in the RYR2 gene is responsible for 50-65 percent of the cases of CPVT. Doctors can easily screen for these mutations in the RYR2 gene by administering a FAMILION-CVPT genetic test[2].
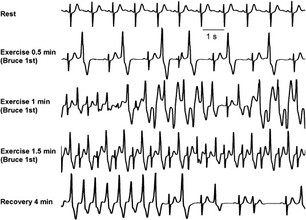
Figure 1: This figure shows the ECG of a patient with CPVT while exercising.
As you can see, as the patient continues to exercise, the premature
ventricular contractions start to develop. As they continue, the arrh-
ythmias become more severe[10].
As you can see, as the patient continues to exercise, the premature
ventricular contractions start to develop. As they continue, the arrh-
ythmias become more severe[10].
Once diagnosed, CPVT is very treatable. Most patients will be inititally prescribed a beta-blocker. If symptoms still persist, this is a sign of incomplete protection of the medication and doctors may prescribe Flecainide, an anti arrhythmic medication as a supplement[2,6]. For patients at risk for ventricular fibrillation or cardiac arrest, an implantable cardioverter defibrillator will be put into the patient. The device has a small computer that monitors the patient's heart beat[2]. If it detects any irregular beating or if it notices fibrillation or cardiac arrest, it will send small electrical pulses to the heart as an attempt to get the heart to contract in unison again[5].
RYR2 Gene
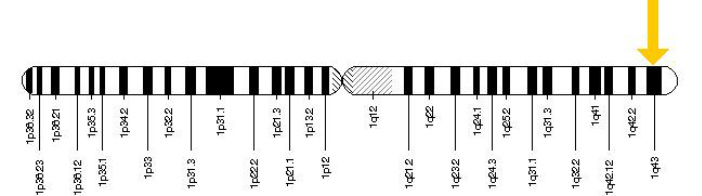
Figure 2: The RyR2 gene is located at on chromosome 1 at location 43 as indicated by the yellow arrow[4].
The RYR2 gene encodes the Ryanodine Receptor 2 protein which acts as the calcium ion channel in the sacroplasmic reticulum membrane of cardiac muscle cells[4,8]. Mutation in the RYR2 gene has been linked to 50-65 percent of CPVT cases[2]. As seen above, in Figure 2 [4],the RYR2 gene is located on chromosome 1 in position 43. The gene itself is 791,778 base pairs long [4] and contains 105 exons or coding regions[7]. Since the discovery of CVPT, over 70 single nucleotide mutations in the RYR2 gene have been linked to the disorder [4]. A single mutation in one base pair in the gene is enough to cause CPVT. Mutations in the gene cause the wrong amino acid to be coded. These missense mutations can disrupt both amino acid interactions within the polypeptide structure as well as protein-protein interactions with other proteins involved in the calcium ion complex. Due to it's defective structure, a mutated Ryanodine Receptor 2 is known to be "leaky" and isn't able to properly regulate the amount of calcium ions that passes through it. An increase of calcium causes cardiac muscle to contract [4]. Cardiac contraction and relaxation is regulated by a combination of different concentrations of sodium, potassium, and calcium ions that create a ion gradient across the myocyte membrane. Leaky Ryanodine Receptor 2 proteins delay the rate of depolarization of the cell and disrupts the pattern that the heart contracts[4,7,8].
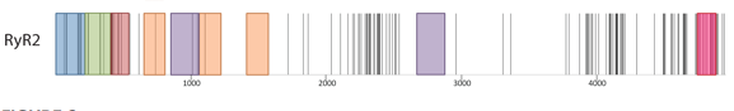
Figure 3: This figure shows in which domains disease causing mutations of the RYR2 gene occur. Each mutation is represented by a vertical black line. Domains are color coded. (A) domain (red), (B) domain (green), (C) domain (red), SPRY domain (orange), Tandem Repeat domain (Purple), and Pore Forming domain (Pink) [3].
|
|
Animation 2 : This animation show's the membrane potential of a myocyte created by sodium, potassium and calcium ions. The Ryr2 gene creates the protein that makes-up the calcium channel. How does a defective calcium channel affect the electrophysiology of the heart[11]. |
References:
[1] Gene Reviews. (2013). Electronic references. Retrieved January 31, 2014, from
http://www.ncbi.nlm.nih.gov/books/NBK1289/
[2]SADS Foundation. (2008). Electronic references. Retrieved February 1, 2014 from
http://www.sads.org/library/cpvt#.UuQigDl6i1s
[3]Paivi J. Laitinen, Kevin M. Brown, Kirsi Piippo, Heikki Swan. (2001). Mutations in Cardiac Ryanodine Receptor (RyR2) Gene
in Familial Polymorphic Ventricular Tachycardia. Circulation. 103. 485-490. doi: 10.1161/01.CIR.103.4.485
http://circ.ahajournals.org/content/103/4/485.full.pdf+html
[4] US. National Library of Medicine. (2009). Electronic References. Retrieved February 1, 2014 from
http://ghr.nlm.nih.gov/gene/RYR2
[5] National Heart, Blood, and Lung Institute. (2011). Electronic References Retrieved January 28, 2014 from
http://www.nhlbi.nih.gov/health/health-topics/topics/icd/howdoes.html
[6]Zhiguang Yuchi, Lynn Kimlicka and Filip Van Petegem (2013). Structural Insights Into Disease Mutations of the Ryanodine
Receptor, Genetic Disorders, Prof. Maria Puiu (Ed.), ISBN: 978-953-51-0886-3, InTech, doi: 10.5772/53641.
http://www.intechopen.com/books/genetic-disorders/structural-insights-into-disease-mutations-of-the-ryanodine-receptor
[7] OMIM. (2011). Electronic References. Retrieved January 28, 2014 from http://www.omim.org/entry/180902
[8]Madame Curie Bioscience Online. (2013). Retrieved February 1, 2014 from
http://www.ncbi.nlm.nih.gov/books/NBK5959/#A37642
[9]https://www.nhlbi.nih.gov/health/health-topics/topics/hhw/contraction.html
[10]http://lifeinthefastlane.com/ecg-library/basics/bvt/
[11]http://highered.mcgrawhill.com/sites/0072948116/student_view0/chapter1/animation_quiz__action_potentials_in_cardia
c_muscle_cells.html
[1] Gene Reviews. (2013). Electronic references. Retrieved January 31, 2014, from
http://www.ncbi.nlm.nih.gov/books/NBK1289/
[2]SADS Foundation. (2008). Electronic references. Retrieved February 1, 2014 from
http://www.sads.org/library/cpvt#.UuQigDl6i1s
[3]Paivi J. Laitinen, Kevin M. Brown, Kirsi Piippo, Heikki Swan. (2001). Mutations in Cardiac Ryanodine Receptor (RyR2) Gene
in Familial Polymorphic Ventricular Tachycardia. Circulation. 103. 485-490. doi: 10.1161/01.CIR.103.4.485
http://circ.ahajournals.org/content/103/4/485.full.pdf+html
[4] US. National Library of Medicine. (2009). Electronic References. Retrieved February 1, 2014 from
http://ghr.nlm.nih.gov/gene/RYR2
[5] National Heart, Blood, and Lung Institute. (2011). Electronic References Retrieved January 28, 2014 from
http://www.nhlbi.nih.gov/health/health-topics/topics/icd/howdoes.html
[6]Zhiguang Yuchi, Lynn Kimlicka and Filip Van Petegem (2013). Structural Insights Into Disease Mutations of the Ryanodine
Receptor, Genetic Disorders, Prof. Maria Puiu (Ed.), ISBN: 978-953-51-0886-3, InTech, doi: 10.5772/53641.
http://www.intechopen.com/books/genetic-disorders/structural-insights-into-disease-mutations-of-the-ryanodine-receptor
[7] OMIM. (2011). Electronic References. Retrieved January 28, 2014 from http://www.omim.org/entry/180902
[8]Madame Curie Bioscience Online. (2013). Retrieved February 1, 2014 from
http://www.ncbi.nlm.nih.gov/books/NBK5959/#A37642
[9]https://www.nhlbi.nih.gov/health/health-topics/topics/hhw/contraction.html
[10]http://lifeinthefastlane.com/ecg-library/basics/bvt/
[11]http://highered.mcgrawhill.com/sites/0072948116/student_view0/chapter1/animation_quiz__action_potentials_in_cardia
c_muscle_cells.html
*** Cover photo credit:http://www.zengardner.com/sacred-language-human-body/
Site created by: Mercede Davis
Email contact: [email protected]
Date last updated: 5/14/14
Genetics 564, University of Wisconsin-Madison
Email contact: [email protected]
Date last updated: 5/14/14
Genetics 564, University of Wisconsin-Madison